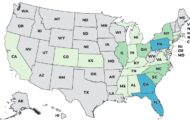
The type of Salmonella making people sick in the Foster Farms chicken outbreak is putting victims in the hospital at an alarming rate, has proven to be resistant to antibiotics and is causing blood infections at an abnormally high rate, according to state and federal infectious disease experts. Foodborne pathogens that are resistant to drug treatment aren’t new, officials say, but the Foster Farms outbreak is a clear example of how food safety is becoming more important.
 “With so many people being treated at hospitals for illnesses related to food poisoning by Foster Farms, this outbreak is showing more and more people what a burden it can be to stack contaminated food into our grocery aisles,” said Fred Pritzker, a food safety lawyer representing victims of the outbreak. Pritzker said 42 percent of case patients in the outbreak, which has hit especially hard in California and the West, have been hospitalized to overcome complications of salmonellosis.
“With so many people being treated at hospitals for illnesses related to food poisoning by Foster Farms, this outbreak is showing more and more people what a burden it can be to stack contaminated food into our grocery aisles,” said Fred Pritzker, a food safety lawyer representing victims of the outbreak. Pritzker said 42 percent of case patients in the outbreak, which has hit especially hard in California and the West, have been hospitalized to overcome complications of salmonellosis.
The Food Safety Inspection Service (FSIS), an arm of USDA, has characterized the hospitalization rate as abnormally high. And in a recent Foster Farms outbreak update released by the Centers for Disease Control and Prevention (CDC), epidemiologists working on the outbreak reported that 13 percent of ill persons have developed blood infections as a result of their illness. “Typically, approximately 5 percent of persons ill with Salmonella infections develop blood infections,” the CDC said.
FSIS and CDC have reported that seven different strains of Salmonella Heidelberg are causing illness in the Foster Farms outbreak. This antibiotic resistance may be associated with the increased risk of hospitalization or possible treatment failure in infected individuals, the agencies have said. “The information collected for cases associated with each strain indicates that each of the strains is linked to this outbreak of multidrug-resistant Salmonella Heidelberg infections and that Foster Farms brand chicken is the likely source,” The CDC said Friday.
NARMS laboratory conducted antibiotic-resistance testing on clinical isolates collected from ten ill persons infected with three of the seven outbreak strains. Nine of these isolates exhibited drug resistance to one or more commonly prescribed antibiotics. Of those, three were multidrug resistant. To date, NARMS reports that isolates collected from ill persons were resistant to combinations of the following antibiotics: ampicillin, chloramphenicol, gentamicin, kanamycin, streptomycin, sulfisoxazole, and tetracycline. Antimicrobial resistance may increase the risk of hospitalization or possible treatment failure in infected individuals, Pritzker said.
NARMS, established in 1996, stands for the National Antimicrobial Resistance Monitoring System for Enteric Bacteria. It is a collaboration among state and local public health departments, CDC, the U.S. Food and Drug Administration and the U.S. Department of Agriculture. This national public health surveillance system tracks changes in the antimicrobial susceptibility of certain enteric (intestinal) bacteria found in ill people, retail meats, and food animals in the United States.
Testing at NARMS will continue as the outbreak continues to unfold. FSIS has said it will continue intensified sampling and testing of chicken products from three Foster Farms manufacturing plants for at least the next 90 days.