The Centers for Disease Control and Prevention (CDC) has released a report titled “Safer Food Saves Lives.” In it, they state that more multistate food poisoning outbreaks are being discovered and reported. Those outbreaks are very serious, even though individual food poisoning cases are more common. In fact, multistate outbreaks caused 56% of all deaths in all reported foodborne outbreaks, even though they accounted for just 3% of all outbreaks from 2010 to 2014.
 In other words, while multistate food poisoning outbreaks are not common, they are more deadly. That’s because the bacteria Salmonella, E. coli, and Listeria monocytogenes cause 91% of multistate outbreaks. Those bacteria can cause serious illness, severe complications such as hemolytic uremic syndrome, and are deadly.
In other words, while multistate food poisoning outbreaks are not common, they are more deadly. That’s because the bacteria Salmonella, E. coli, and Listeria monocytogenes cause 91% of multistate outbreaks. Those bacteria can cause serious illness, severe complications such as hemolytic uremic syndrome, and are deadly.
On average, there have been about 24 multistate outbreaks every year in the last five years. That is an increase of 25% over the past thirty years. And each outbreak involves from 2 to 37 states. Forty-six percent of multistate foodborne outbreaks result in product recalls, such as the Blue Bell ice cream Listeria monocytogenes outbreak last summer, or the Salmonella outbreak linked to recalled Barber Foods and Aspen Foods frozen chicken products.
Investigations of these outbreaks have found food safety issues on the farm, in distribution, in processing, and in preparation. Outbreaks have ranged from illnesses caused by a single item, such as recalled sprouts or ground beef, or larger more complex outbreaks linked to an event or single facility such as a restaurant.
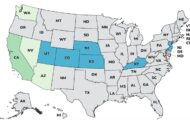
The current ongoing outbreak at Chipotle restaurants in the Northwest United States is a case in point. At least 41 people are sick with E. coli infections in Oregon and Washington after eating at those restaurants. That means it’s likely that food purchased from a large scale distributor was contaminated. The chain purchased the food and distributed it to their 43 restaurants in those two states. It was served to customers, and they got sick.
The government thinks that the increase in multistate outbreaks may be because of large-scale suppliers covering more distribution areas. Restaurant chains and grocery stores use large suppliers who purchase food from many growers and ship it across the country. That means that if some lettuce grown in Arizona is contaminated, it could sicken people across the country after being sold in grocery stores and restaurants.
These outbreaks are difficult to solve precisely because there are so many moving parts. People in many states getting sick from a contaminated food means public health officials have to interview all of the patients, discover a common thread, then trace that thread back to the farm or distribution center to find the pathogenic bacteria source. It’s difficult to remember what you ate yesterday, let alone weeks or months ago, so that information is unreliable and hard to come by. And if a single food is contaminated, people may eat it in many different foods.
Companies may not have complete records about where the food they distributed came from, making traceback investigations even more difficult. Many different farms can produce the beef sold in a single burger or vegetables sold in one crate. Imported foods can be even harder to trace, and the number of foods imported into this country is increasing.
Foods that we don’t think of as being a food safety risk have been the causes of serious outbreaks recently, complicating matters further. The Listeria monocytogenes outbreak linked to Bidart Brothers caramel apples in the fall of 2014was unexpected, as was the Salmonella outbreak in 2014 linked to organic chia powder.
But outbreak discoveries may be becoming more common because technology is getting more sophisticated. PulseNet, the national lab that collects bacterial DNA from ill persons, lets investigators find people who were sickened with the same bacteria, down to its DNA, identifying outbreaks that may have gone unnoticed in earlier years.
The Listeria monocytogenes outbreak linked to Karoun Dairies soft cheeses, for example, was discovered this year. It was unusual because the products sickened 24 people over a five year period. Investigators noticed that a few were sickened with the same strain of Listeria. Further investigating uncovered the 24 patients through the PulseNet system. Those patients were interviewed and it was revealed they ate Karoun Dairies unusual cheeses before getting sick. Then, environmental samples taken from Karoun Dairies found bacteria with nearly identical DNA. Without the bacteria DNA database, that outbreak would not have been solved.
The government and food industries need to work together to make food safer. Better methods to detect and investigate outbreaks will help, but corporations need to have HACCP plans, keep good records, and insist on food safety priority from the vendors they use.
The CDC offers an infographic detailing how outbreaks begin and how public health officials solve them. While there are only three basic steps that can lead to an outbreak, there are at least nine steps to solve one.