Idaho health officials believe a raw milk outbreak that began in early October has ended after sickening 12 people. Two people were hospitalized.
Idaho health officials believe a raw milk outbreak that began in early October has ended after sickening 12 people. Two people were hospitalized.
Four people who drank raw milk from Natural Farm Fresh Dairy in Kuna developed E. coli O157: H7 infections and four people developed Campylobacter infections. Four others had symptoms consistent with food poisoning.
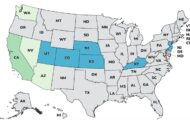
The Campylobacter and E. coli cases, in Ada and Canyon counties, were reported by the Idaho Department of Health on October 20. No new illness have been reported in 10 days.
The Idaho Department of Agriculture did not find bacteria in the milk it tested. However, milk it tested was not from the batch that made people sick. Agriculture officials inspected the dairy Tuesday morning. The dairy, which suspended operations during the investigation, met all criteria and has begun production again.
In the announcement of the outbreak, Idaho health officials urged consumers to educates themselves about the dangers of raw milk, a common source of food poisoning. In 2013, 85 percent of dairy outbreaks were attributed to raw milk products, according to the Centers for Disease Control and Prevention (CDC).
Those at higher risk of illness after consuming unpasteurized milk include children, pregnant women, the elderly, and those with compromised immune systems. Children are disproportionately affected by raw milk outbreaks, often they account for the majority of case patients.
Campylobacter and E.coli are bacteria that live in the intestines of animals and are shed in their feces. They are transmitted via the fecal-oral route, meaning people ingest food or drinks that are contaminated with microscopic amounts of fecal matter.
Campylobacter is the most common source of raw milk outbreaks such as the May outbreak in Indiana that sickened several children in the Odon and Montgomery areas; a March outbreak that sickened several people in Northern California; and an October 2014 outrbeak in Durand, Wisconsin.
Common symptoms of campylobacteriosis include fever, diarrhea that is sometimes bloody, abdominal cramps and vomiting. Symptoms usually begin two to five days after exposure and last for about a week. For about 20 percent of people with these infections, symptoms can last for up to three weeks. In some cases, a Campylobacter infection can cause Guillain-Barré syndrome, an illness that causes paralysis and death.
E. coli O157:H7 symptoms include stomach cramps and diarrhea that can be bloody. Symptoms usually develop one to four days after exposure and last as long as 10 days. Antibiotics should not be used to treat E. coli infections as they can make the illness worse, according to the CDC.
E. coli O157:H7 infections sometimes lead to a serious complication called hemolytic uremic syndrome (HUS), which can cause kidney failure, seizure, stroke, coma and death. HUS, which often targets children, usually occurs a week or more after the onset of diarrhea.
Because of its frequent association with illness, raw milk is considered a “high risk” food and a public health hazard by the CDC and other public health agencies. They advise that the safest milk products are those that have been pasteurized.