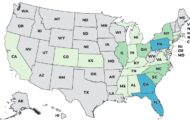
Twenty one people in eight states are sick with multidrug-resistant Salmonella Heidelberg infections linked to contact with Dairy Bull Calves, according to the Centers for Disease Control and Prevention. Epidemiologic, traceback, and laboratory results linked this outbreak to contact with the calves that were purchased from livestock markets in Wisconsin.

Eight of those sickened have been hospitalized. No deaths have been reported. Among 19 people with available information, illnesses began on dates ranging from January 11, 2016 to October 24, 2016. The patient age range is from less than 1 year to 72, with a median age of 21.
PulseNet was used to identify people who may be part of this outbreak. PulseNet performs DNA fingerprinting on bacteria with pulsed field-gel electrophoresis (PFGE) and whole genome sequencing (WGS). A national database of this data is maintained to help identify these outbreaks.
Isolates from ill people are closely related, according to whole genome sequencing. That means that people in this outbreak are more likely to share a common source of infection.
Dairy bull calves are young, male cattle that have not been castrated and may be raised for meat. Some of the calves in this outbreak have been purchased for use with 4H projects.
In interviews, patients answered questions about contact with animals and the food they ate the week before they got sick. Of the 19 people interviewed, 15, or 79%, reported contact with these animals or other cattle. Some of the ill persons said they got sick after their dairy bull calves became ill or died.
One patient’s dairy calves tested positive for Salmonella Heidelberg. Testing using whole genome sequencing found that isolates from ill people are closely related genetically to isolates from those calves. That means the human infections in this particular outbreak are likely linked to ill calves.
The Wisconsin State Laboratory of Hygiene conducted antibiotic resistance testing on clinical isolates from these patients. The isolates were resistant to antibiotics and shared the same DNA fingerprints. WGS also identified multiple antimicrobial resistance genes in isolates from fifteen patients and eight cattle. All of the isolates were multidrug resistant. This is associated with increased risk of hospitalization, development of a bloodstream infection, or treatment failure.
The symptoms of a Salmonella infection include nausea, vomiting, abdominal pain, diarrhea that may be bloody, fever, chills, headache, and muscle pain. Symptoms usually begin six to seventy-two hours after exposure to the pathogenic bacteria. Most people recover within a week, but some become so ill they must be hospitalized.
The typical hospitalization rate for Salmonella illnesses is about 20%. The hospitalization rate in this outbreak is 38%, almost twice that rate. The fact that the bacteria are resistant to antibiotics and the fact that some of the patients are very young may play a part in that high rate.
To prevent illness from contact with these animals and other animals, follow these steps. Always wash your hands thoroughly with soap and water after touching livestock, equipment used for animals, or anything in the area where the animals live and roam. This is especially important before preparing or consuming food or drinks for others or yourself.
Always use dedicated clothes, shoes, and work gloves when working with livestock. Keep and store these items outside of your house. And work with your veterinarian to keep your animals healthy.