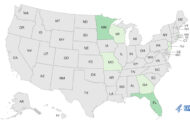
Fourteen people in six states are sickened with E coli 0145; the same strain killed a New Orleans toddler last week. While no one source has been pinpointed, state officials are working with the Centers for Disease Control (CDC) to solve the case and epidemiologists suspect food may be the culprit.
 The case count is as follows:
The case count is as follows:
- Alabama (2)
- California (1)
- Florida (1)
- Georgia (5)
- Louisiana (3 ill, 1 death)
- Tennessee (1)
The CDC has released a statement about the outbreak. They say that the most recent report of illness was on June 4, 2012. The dates when patients became sick range from April 15 to May 12, 2012. Three people have been hospitalized.
Public health officials interview victims with questionnaires, asking them about exposure to different foods, restaurants, animals, and other potential bacterial sources. A petting zoo has been eliminated as the cause of the outbreak.
Food safety experts agree that it’s important to release information about these illnesses, because if someone is experiencing symptoms of E. coli infection, they need to see a doctor and be tested for the bacteria. Each patient is an important link when trying to identify a source of the contamination; information from just one person could solve the case. Patients usually develop STEC infection symptoms within two to eight days after consuming the bacteria.
Symptoms of E. coli infection include a mild fever, severe abdominal and stomach cramps, diarrhea which is often bloody, and vomiting. In some cases, especially children under the age of 5, an E. coli infection can lead to hemolytic uremic syndrome (HUS), a severe condition that can cause kidney failure.
Dr. Raoult Ratard, state epidemiologist with the Louisiana Department of Health and Hospitals, released a statement that said, “The best prevention is always to handle and prepare food in a manner that minimizes the presence of harmful germs.” The statement from LDHH also said that foodborne illnesses are “often discounted by the general public as benign, but this is a reminder that they can have extremely serious consequences.”
Consumers can protect themselves against E. coli infections up to a point. Cross-contamination occurs easily, but by cooking meat thoroughly, washing fruits and vegetables before peeling and slicing, and washing your hands after using the bathroom you can reduce the risk of infections. Avoid raw milk, raw milk products, unpasteurized juice, and undercooked beef. Be careful when handling raw meat. Do not let raw meat juices drip onto other foods and do not put cooked meat on platters that held raw meat. And always use a food thermometer when cooking meat, poultry, eggs, and fish.
E. coli infections tend to spike in the warm weather months because animals shed more of the bacteria at this time. And more people cook hamburgers and steaks on the grill in the summer and may not cook hamburgers to well done, or 165 degrees F. Cross-contamination, either through improper hand washing or contact with raw meat, is another major source of infection in the summer months.