As gross as it may sound, an old method for treating dangerous intestinal infections is being studied. Research on fecal transplants done in the Netherlands was published in the New England Journal of Medicine this month. Doctors in the U.S. first tried this unorthodox treatment in 1958 to treat patients with life-threatening pseudomembranous enterocolitis (colitis).
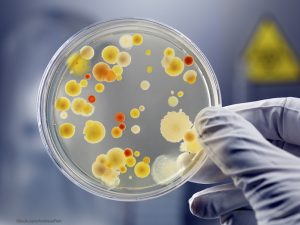 This unconventional treatment involves feces from a healthy donor transplanted into the intestines of patients with these serious infections. The study looked at sixteen people who had recurring infections of Clostridium difficile. After transplant, 15 of the 16 were cured. Among those with the same infection treated with antibiotics, only 3 of 13 and 4 of 13 patients were cured. The healthy bacteria from the donor feces colonizes the intestines of the ill person, successfully controlling C. difficile growth.
This unconventional treatment involves feces from a healthy donor transplanted into the intestines of patients with these serious infections. The study looked at sixteen people who had recurring infections of Clostridium difficile. After transplant, 15 of the 16 were cured. Among those with the same infection treated with antibiotics, only 3 of 13 and 4 of 13 patients were cured. The healthy bacteria from the donor feces colonizes the intestines of the ill person, successfully controlling C. difficile growth.
C. difficile infections kill about 14,000 people every year in this country. Strangely, the infection is caused by antibiotic use, which kill healthy bacteria that live in your intestines. With less competition, C. difficile can easily take hold in patient’s intestines and cause inflammation and severe diarrhea, which can lead to dehydration and death. About 25% of patients with this infection have a recurrence after initial treatment with antibiotics. After the second recurrence, 50% of patients will continue to develop this infection.
The bacteria is found in most hospitals, where it spreads easily through fecal contamination. Hospital toilets are a prime source of microorganisms, especially those which form spores, such as C. difficile. Surfaces such as blood pressure cuffs, IV poles, tables, and bedrails are then easily contaminated with the bacteria by touch. Inadequate cleaning exacerbates the problem.
This study is the first to examine stool transplants in a randomized, controlled study. Although the study was not blinded, meaning researchers knew who received the fecal transplant and who received antibiotics, the findings are statistically significant and important. Natural revulsion towards this type of therapy has been a serious impediment to its study. The study’s authors hope that in the future, “defined mixtures of cultured bacteria that confer colonization resistance against C. difficile” can be used instead of stool transplants.
And there is another significant finding in this study: an increased interest in the study of the microbiome, or collection of bacteria, that live in our intestines. In the future, doctors may be able to affect our health and treat diseases by manipulating intestinal microbes without having to use antibiotics or other conventional treatments.



Same here Howard, my sister’s life was saved by fecal microbiota transplant – she had c-diff and nearly died. There is also lots of information at http://www.fecalmicrobiotatransplant.com – including a medical report about how FMT has brought about long term continuing remission of over 15 years of MS in three patients treated for constipation (as one of the complications of multiple sclerosis. This is the tip of the iceberg!
A fecal transplant (FT) pretty much saved my uncle’s life. He had the C. diff colitis infection and was in progressive decline. About 4 days after the FT he started feeling normal again…. get the word out!
Visit my advocacy blog for more information at http://fecaltransplant.info
or www [dot] fecaltransplant [dot] info