 Identifying the contaminated food source responsible for a food poisoning outbreak isn’t always as straightforward as it seems, especially when perishable items are involved. A short shelf life means evidence often is either eaten or thrown away before an investigation even gets started. That’s the case with the Chipotle E. coli outbreak.
Identifying the contaminated food source responsible for a food poisoning outbreak isn’t always as straightforward as it seems, especially when perishable items are involved. A short shelf life means evidence often is either eaten or thrown away before an investigation even gets started. That’s the case with the Chipotle E. coli outbreak.
Health officials suspect that contaminated produce is the source of the outbreak. But it’s likely that the tainted batch was consumed before investigators gathered samples from restaurants for testing as is often the case. The first round of tests on samples taken from several Chipotle restaurants were negative for the outbreak strain E. coli O26. Other tests are pending.
It’s important to note that finding the outbreak strain in uneaten food is not a necessary component of an outbreak investigation. In fact, it doesn’t happen often. When health investigators have food histories, traceback information and epidemiologic evidence, that’s enough to determine the source of the outbreak.
Chipotle didn’t dispute that fact. The company took responsibility, apologized and is making changes to prevent future problems. But that’s not how all food producers act.
Recent examples of companies initially operating from the “it wasn’t us” stance include Andrew & Williamson (cucumbers), Foster Farms (chicken), Blue Bell, (ice cream), Aspen Foods (frozen breaded chicken), and just about every producer of unpasteurized beverages (apple juice, raw milk). But a common food source or common facility is enough to apportion blame. Here’s why.
Food histories. When 12 people get sick and the only thing all of them ate was Food A, that’s a good indication that something is wrong with Food A.
If the illness was caused by E. coli, Listeria or Salmonella bacteria, DNA tests can be performed on samples from patients. These tests identify specific fingerprints. When samples from sick consumers produce matching E. coli fingerprints, it means they were sickened by the same source. And if the only thing they all ate was Food A, again, it is a clear indication that something is wrong with Food A.
Sometimes companies implicated in outbreaks will say “you can get E coli/Listeria/Salmonella from lots of things.” That’s true. But what’s also true is that the E. coli on Food A is different, and looks different under a microscope, than the E. coli on Food B.
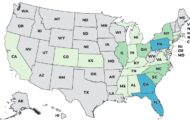
State and federal investigators are continuing the investigation of the outbreak which has sickened 42 people so far, 27 in Washington and 15 in Oregon. Fourteen people have been hospitalized.
In Washington, the 27 cases were reported. Tests on an additional four cases are pending. The confirmed cases were reported from the following counties: Clark (11), Cowlitz (2), Island (2), King (6), Skagit (5), and Whatcom (1). Ten of these people were hospitalized. None of them developed Hemolytic Uremic Syndrome (HUS), a complication that arises in about 15 percent of E. coli cases that causes kidney failure.
The E. coli strain in this outbreak, E. coli O26, produces shiga toxins that can cause severe, life-threatening illness which can, in some cases, be fatal. Symptoms include bloody diarrhea, abdominal cramps, fever, and vomiting. Anyone with these symptoms should see a doctor.




It is incorrect to say that this outbreak could be caused by an employee who didn’t wash their hands after using the restroom. The strain of e.coli identified is e.colo O26 which resides in the gut of cattle. Also, the investigation of all the chipotle stores involved has revealed no evidence of e.coli in any of the produce that was available for testing. Last night they had ruled out produce as a source of contamination. While it is difficult to determine a source of a contaminate in fresh food, as they have a short shelf life and are usually gone by the time the investigation begins, there is usually some trace of the organism in storage containers, etc. Nothing like this has been found, so product is an unlikely cause.
Sorry for the typo above, but my phone won’t let me go back and correct it.
That’s not quite true. Some people can carry the E. coli bacteria, even the O26 strain, and not show symptoms. And if someone had an E. coli infection, they can shed the bacteria for several months after recovering. If they are shedding the bacteria in their feces, they could pass it on to others after improper bathroom hygiene.
And even though no E. coli bacteria was found in the produce tested doesn’t mean there was no E. coli in any of the produce Chipotle sold. As the story explains, the evidence may have been consumed or thrown out. In addition, there is no way to test every milliliter of every food item sold, or every inch of every container that held food.
Many food poisoning outbreaks go unsolved, that is, the outbreak strain of the bacteria are not found in a suspected food source.